Table of Contents
Vitamin D is often celebrated as the “sunshine vitamin”—essential for strong bones, immunity, and overall health. In recent years, awareness about vitamin D deficiency has increased worldwide, including in South Asia. As a result, supplements are widely prescribed and easily available.
But there is an important question many people overlook:
Can you take too much vitamin D?
The answer is yes. Although vitamin D deficiency is common, excessive intake can lead to vitamin D toxicity, a potentially serious medical condition.
What Is Vitamin D Toxicity?
Vitamin D toxicity (hypervitaminosis D) occurs when excessive amounts of vitamin D accumulate in the body, leading to dangerously high levels of calcium in the blood (hypercalcemia).
Unlike many water-soluble vitamins, vitamin D is fat-soluble, meaning it is stored in the body and not easily excreted. Excess intake over time can therefore cause toxic buildup.
Importantly, vitamin D toxicity almost never occurs from sunlight exposure. It is almost always due to overuse of supplements.
Why Is Vitamin D Important?
Vitamin D plays several key roles in the body:
- Enhances intestinal absorption of calcium and phosphorus
- Maintains bone mineralization
- Supports muscle function
- Contributes to immune regulation
- May influence cardiovascular and metabolic health
Because of these benefits, vitamin D supplements are frequently recommended. However, more is not always better.
Causes of Vitamin D Toxicity
The most common cause is excessive supplementation.
Common scenarios include:
- High-dose vitamin D injections taken frequently
- Taking multiple vitamin supplements simultaneously
- Prescribing high doses for prolonged periods without monitoring
- Medication errors or incorrect dosing
- Self-medication with over-the-counter supplements
Vitamin D toxicity usually occurs when daily intake exceeds 10,000 IU for several weeks or months, although susceptibility varies among individuals.
How Does Vitamin D Toxicity Harm the Body?
Vitamin D increases calcium absorption from the gut. When vitamin D levels become excessively high, this leads to hypercalcemia.
High calcium levels can damage several organs:
- Kidneys → kidney stones, nephrocalcinosis, renal failure
- Heart → arrhythmias
- Brain → confusion, lethargy
- Gastrointestinal tract → nausea, vomiting, constipation
In severe cases, toxicity can become life-threatening.
Symptoms of Vitamin D Toxicity
Symptoms are mainly due to hypercalcemia and may develop gradually.
Early symptoms
- Loss of appetite
- Nausea and vomiting
- Constipation
- Fatigue and weakness
- Excessive thirst (polydipsia)
Later symptoms
- Frequent urination (polyuria)
- Dehydration
- Abdominal pain
- Muscle weakness
- Confusion or altered mental status
Severe complications
- Kidney stones
- Acute kidney injury
- Cardiac arrhythmias
- Calcification of organs
Diagnosis
Diagnosis is based on clinical suspicion and laboratory findings.
Key investigations
| Test | Expected Finding |
|---|---|
| Serum 25-hydroxyvitamin D | Usually >150 ng/mL |
| Serum calcium | Elevated |
| Serum phosphorus | Often elevated |
| Parathyroid hormone (PTH) | Suppressed |
| Serum creatinine | May be elevated |
| Urinary calcium | Increased |
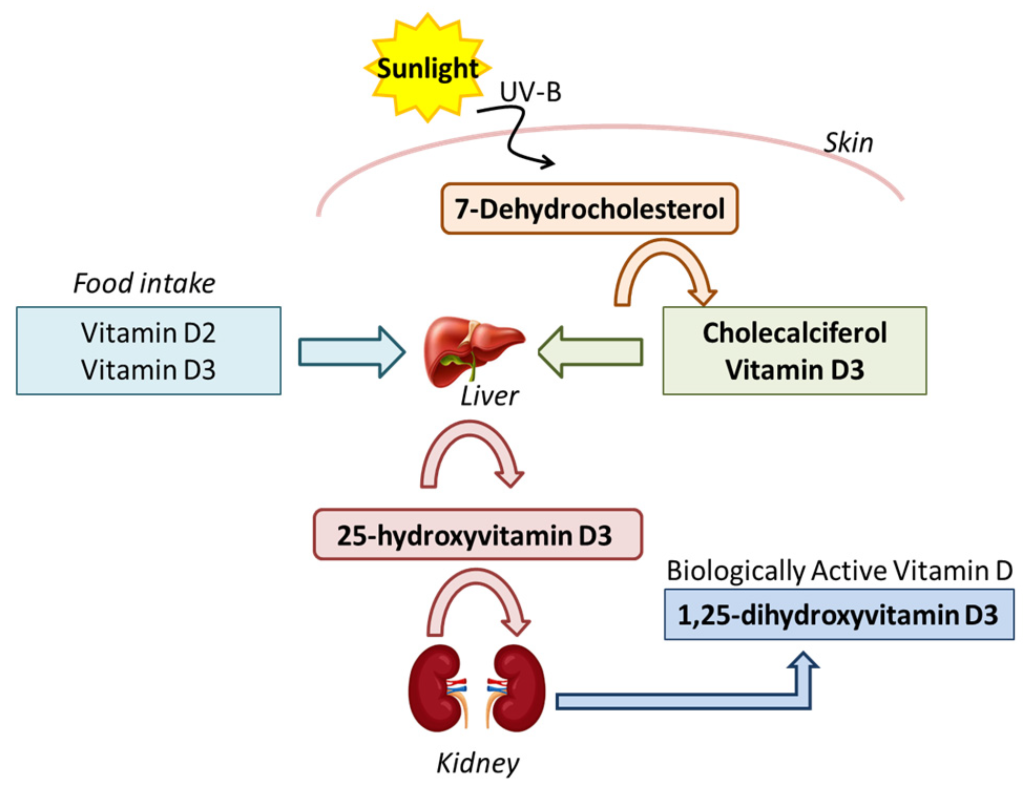
The best marker of vitamin D status is serum 25-hydroxyvitamin D.
Treatment of Vitamin D Toxicity
Management focuses on reducing calcium levels and stopping vitamin D exposure.
Immediate steps
- Stop vitamin D and calcium supplements
- Hydration with intravenous fluids
- Promote calcium excretion
Medications used
- Loop diuretics (after hydration)
- Corticosteroids
- Bisphosphonates
- Calcitonin (in severe hypercalcemia)
Severe cases may require hospital admission.
Safe Vitamin D Intake
Recommended daily intake varies by age.
| Age Group | Recommended Intake |
|---|---|
| Infants | 400 IU/day |
| Children | 600 IU/day |
| Adults | 600–800 IU/day |
The upper safe limit for adults is generally considered 4,000 IU/day unless supervised by a doctor.
High-dose therapy (e.g., 60,000 IU weekly) should only be taken under medical supervision.
Prevention: The Key Message
Vitamin D toxicity is rare but entirely preventable.
Safe practices include:
- Avoid self-medication with high-dose supplements
- Follow doctor-recommended dosing
- Monitor vitamin D levels during prolonged therapy
- Avoid combining multiple vitamin D products
Remember: supplements are medications, not harmless vitamins.
Final Thoughts
Vitamin D is essential for health, but balance is crucial. In the era of widespread supplementation, awareness of vitamin D toxicity is increasingly important for both patients and healthcare providers.
Adequate sunlight, balanced nutrition, and appropriate supplementation under medical guidance are the safest ways to maintain optimal vitamin D levels.
Because even the sunshine vitamin can cast a shadow when taken in excess.






Leave a Reply